Why Practices, Clinics, and Healthcare Organizations Need Financial Leadership
Healthcare organizations are built to care for people. But behind every successful practice, clinic, medical group, or healthcare nonprofit is another system that must work just as reliably: the financial system.
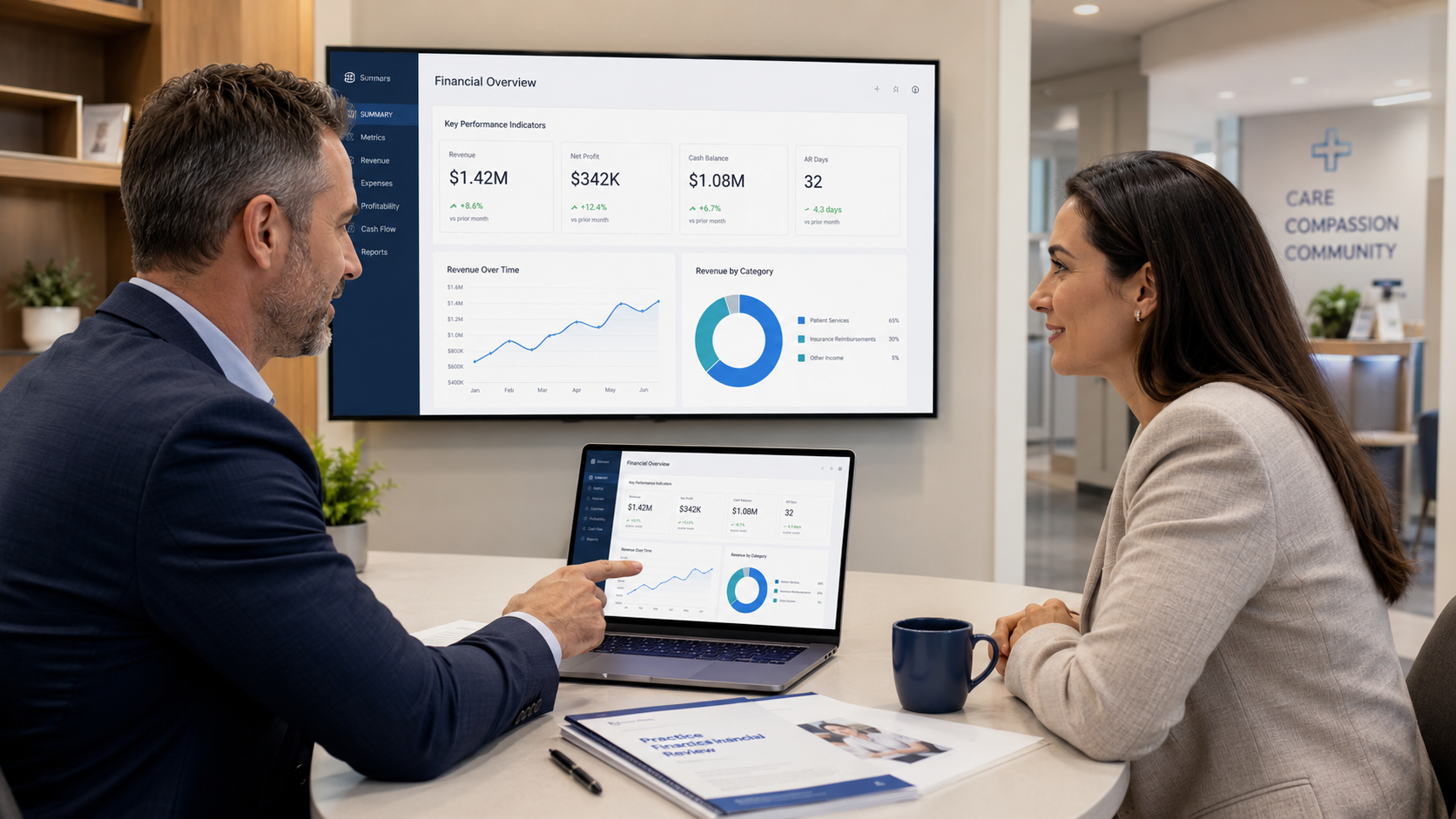
Why Practices, Clinics, and Healthcare Organizations Need Financial Leadership

Healthcare organizations are built to care for people. But behind every successful practice, clinic, medical group, or healthcare nonprofit is another system that must work just as reliably: the financial system.
When the financial side is weak, the entire organization feels it.
Reports arrive late. Cash flow becomes difficult to predict. Billing data lives in one system, payroll in another, expenses in another, and leadership is forced to make decisions from spreadsheets that may or may not be accurate.
For a small medical practice, that can mean not knowing whether growth is actually profitable. For a multi-location clinic, it can mean struggling to understand which location is performing well and which one is quietly draining margin.
For a larger healthcare organization, it can mean board meetings, lender conversations, grant reporting, and strategic planning are built on incomplete financial visibility.
That is why healthcare organizations need financial leadership, not just bookkeeping, accounting, or basic reporting.
Financial leadership gives healthcare leaders the ability to understand what is happening, why it is happening, and what to do next.
Financial Leadership Is More Than Accounting
Accounting tells you what happened.
Financial leadership helps you decide what should happen next.
That distinction matters.
A healthcare organization may have someone reconciling accounts, paying bills, producing financial statements, and tracking expenses. Those functions are important. But they do not automatically create leadership-level insight.
Financial leadership connects the numbers to the operation.
It answers questions like:
What services are most profitable?
Which locations are underperforming?
Are staffing costs aligned with patient volume?
Is reimbursement timing creating cash pressure?
Are we growing revenue while losing margin?
Can leadership trust the numbers before making decisions?
Is the organization ready for a new ERP system, new location, new service line, or acquisition?
Without that level of financial visibility, leaders often operate reactively. They solve problems after they become expensive instead of identifying risks early.
Healthcare Finance Is More Complex Than Most Industries
Healthcare organizations face a unique mix of operational, financial, and compliance pressure.
A retail business may sell a product and collect payment immediately. A healthcare organization often delivers care first, then waits for reimbursement through payers, patients, government programs, grants, contracts, or patient balances.
That creates financial complexity.
Revenue does not always equal cash. Patient volume does not always equal profitability. Growth does not always equal stability.
A clinic can look busy and still struggle financially. A practice can increase visits and still lose money if reimbursement, staffing, coding, billing, denials, supply costs, or overhead are not being managed properly.
This is why healthcare financial management requires more than general accounting. It requires a leader who understands how finance connects to operations, systems, reporting, cash flow, and long-term strategy.
Small Practices Need Financial Leadership Too
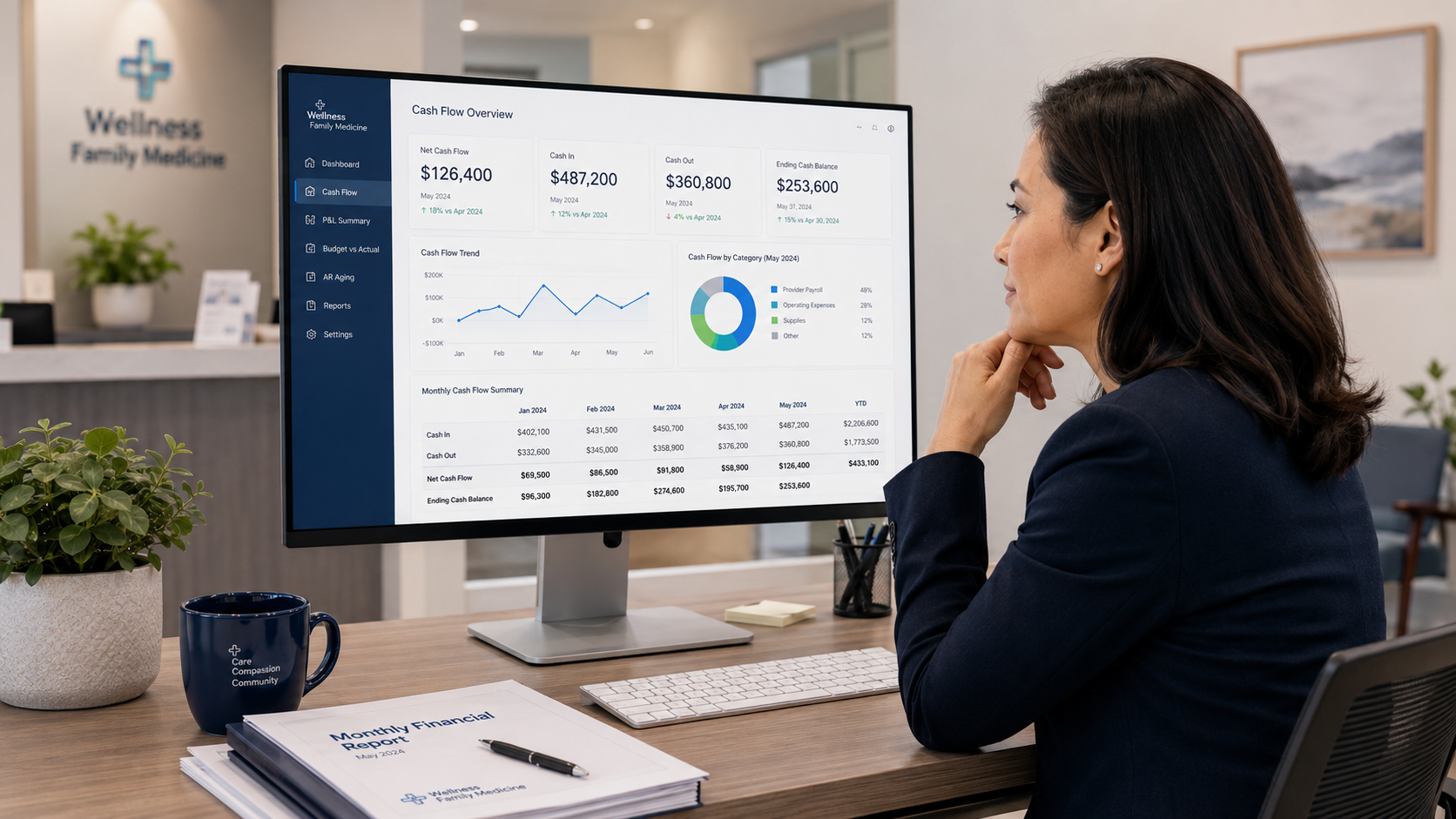
Small practices often need financial leadership even more because the margin for error is smaller.
A few missed billing issues, delayed reconciliations, uncontrolled expenses, or poor cash flow decisions can create serious pressure. The owner may be focused on patient care, staffing, operations, and growth while trying to interpret financial reports that are too late or too limited to guide real decisions.
For smaller practices, financial leadership can help with:
Monthly financial review
Cash flow planning
Budgeting and forecasting
Expense control
Provider productivity analysis
Revenue cycle visibility
Pricing and reimbursement review
Staffing and payroll alignment
Financial dashboards
Profitability by service line
Planning for growth, acquisition, or succession
The goal is not to make finance more complicated. The goal is to make it clear enough that the owner or administrator can lead with confidence.
Clinics Need Better Visibility Across Operations
Clinics often sit in the middle.
They may be too complex for basic bookkeeping but not large enough to justify a full internal CFO team.
That is where financial leadership becomes especially valuable.
A clinic needs to understand how patient volume, staffing, payer mix, reimbursements, supply costs, rent, technology, and administrative overhead work together.
Without strong reporting, leadership may know the clinic is busy but not know whether it is financially healthy.
A clinic may need answers to questions like:
Are we collecting fast enough?
Are denials increasing?
Are certain services producing low margins?
Are labor costs rising faster than revenue?
Are we overstaffed during slow periods?
Are we underinvesting in profitable service lines?
Are reports available early enough to make decisions?
Are our systems creating duplicate work?
Financial leadership turns these questions into a structured operating rhythm. That rhythm allows clinic leaders to review the right numbers every month, spot trends early, and make better decisions before problems compound.
Larger Healthcare Organizations Need Strategic Financial Infrastructure
For larger healthcare organizations, the issue is not usually whether finance exists. The issue is whether finance is structured well enough to support leadership decisions.
A growing healthcare organization may already have accountants, controllers, billing teams, department managers, and software systems. But if those systems are disconnected, reporting may still be slow, inconsistent, or difficult to trust.
This creates major leadership problems.
Boards need reliable financial packages. Executives need forward-looking forecasts. Department leaders need performance dashboards. Finance teams need clean month-end close processes. Investors, lenders, donors, or grantors may need accurate reporting.
At scale, weak financial infrastructure creates drag.
It slows decisions. It increases risk. It burns staff time. It creates confusion between departments. It makes strategic planning harder.
Financial leadership helps larger organizations build the structure needed for scale:
Cleaner month-end close
Standardized reporting packages
ERP implementation or optimization
Department-level financial accountability
Budgeting and forecasting discipline
Cash flow visibility
KPI dashboards
Board-ready financial reporting
Internal controls
Process automation
Leadership does not just need more data. Leadership needs better financial architecture.
The Spreadsheet Problem in Healthcare
Spreadsheets are useful tools. But they become dangerous when they become the financial operating system of the organization.
Many healthcare organizations rely on spreadsheets because they are flexible, familiar, and easy to build quickly. Over time, those same spreadsheets become fragile, disconnected, and difficult to audit.
The warning signs are easy to spot:
Only one person understands the spreadsheet.
Numbers change depending on who prepared the report.
Reports require manual copying and pasting from multiple systems.
Leadership receives reports too late to act.
There is no single source of truth.
Month-end close takes too long.
Budgeting is disconnected from actual performance.
Different departments use different numbers.
In healthcare, this problem can become especially painful because billing, payroll, clinical operations, scheduling, grants, payer contracts, and expenses may all live in separate systems.
Financial leadership helps replace spreadsheet dependency with structured reporting, better workflows, and systems that produce more reliable information.
ERP and Financial Systems Matter
Healthcare organizations do not need technology for the sake of technology. They need systems that support better decisions.
An ERP or financial management platform should help leadership understand the organization faster and more accurately. But many ERP projects fail to deliver that value because the implementation is treated as a software project instead of a finance transformation project.
The system may go live, but the reporting is weak. Data may migrate, but workflows remain messy. Dashboards may exist, but they do not answer the questions leadership actually has.
Financial leadership helps connect ERP decisions to business outcomes.
Before implementing or optimizing an ERP system, healthcare leaders should ask:
What decisions should this system help us make?
What reports do leaders need every month?
What data must be clean before migration?
What workflows should be simplified before implementation?
What manual processes should be eliminated?
What financial controls need to be built into the system?
What KPIs should be visible by location, department, provider, or service line?
The right ERP system should reduce confusion, not create another layer of complexity.
The Month-End Close Is a Leadership Issue
Month-end close is often treated as an accounting task.
It is actually a leadership issue.
If the financial close takes too long, leadership is always looking backward. By the time reports are ready, the organization may already be weeks into the next month.
That delay affects decisions.
A healthcare organization cannot manage cash flow, staffing, expenses, payer issues, or growth effectively if financial information is late.
A strong close process should produce timely, accurate, decision-ready reporting. It should also reduce manual work, improve accountability, and create consistency from month to month.
Financial leadership helps answer:
How long does close currently take?
Where are the bottlenecks?
Which reconciliations are manual?
Which reports are most important?
Which numbers are frequently adjusted?
Which systems are not connected?
Who owns each part of the close process?
The goal is not simply to close faster. The goal is to give leadership reliable information while it is still useful.
Healthcare Leaders Need KPIs They Can Actually Use
Not every metric is a leadership metric.
Healthcare organizations can drown in data and still lack insight.
The right KPIs should help leaders understand performance, risk, cash flow, efficiency, and profitability. They should be reviewed consistently and tied to decisions.
Useful healthcare finance KPIs may include:
Days cash on hand
Net collection rate
Denial rate
Accounts receivable aging
Revenue by service line
Revenue by provider
Revenue by location
Labor cost as a percentage of revenue
Patient volume trends
Operating margin
Budget versus actual performance
Cash flow forecast
Month-end close timeline
Grant or restricted fund reporting, if applicable
The best financial leaders do not just create dashboards. They help leaders understand which numbers matter, why they matter, and what action should follow.
Fractional CFO Support Can Fill the Leadership Gap
Not every healthcare organization needs a full-time CFO.
But many need CFO-level thinking.
That is where fractional CFO support can be a powerful fit.
A fractional CFO gives practices, clinics, and healthcare organizations access to strategic financial leadership without the cost of a full-time executive hire.
This can be especially valuable for:
Growing medical practices
Multi-location clinics
Healthcare nonprofits
Specialty practices
Founder-led healthcare businesses
Organizations preparing for ERP implementation
Organizations with delayed or unreliable reporting
Organizations that need board or lender-ready financials
Organizations that have outgrown basic bookkeeping
The right fractional CFO does not replace the accounting team. Instead, they help elevate the finance function so leadership can make better decisions.
Financial Leadership Improves Decision-Making
Healthcare leaders make important decisions every day.
Should we hire?
Should we open another location?
Should we expand a service line?
Should we renegotiate payer contracts?
Should we invest in new technology?
Should we cut costs?
Should we change staffing models?
Should we pursue financing?
Should we merge, acquire, or sell?
Each of these decisions has financial consequences.
Without strong financial leadership, leaders may rely on instinct, incomplete reports, or delayed information. With strong financial leadership, they can make decisions with clearer visibility into risk, return, timing, and operational impact.
That does not mean every decision becomes easy. It means decisions become better informed.
Financial Leadership Builds Trust
Financial clarity builds trust.
Executives trust the numbers.
Boards trust the reporting.
Managers trust the dashboards.
Lenders trust the financial package.
Grantors trust the documentation.
Owners trust the direction of the business.
Employees benefit from a more stable organization.
Patients benefit when the organization can invest wisely, operate efficiently, and sustain care delivery.
In healthcare, financial leadership is not just about profit. It is about sustainability, accountability, and the ability to continue serving people well.
Warning Signs Your Healthcare Organization Needs Financial Leadership
A practice, clinic, or healthcare organization may need stronger financial leadership if any of the following are true:
Financial reports are consistently late.
Leadership does not fully trust the numbers.
Cash flow feels unpredictable.
Month-end close takes too long.
The organization depends heavily on spreadsheets.
No one can clearly explain profitability by service line, provider, or location.
Budgeting feels disconnected from reality.
The finance team is always reacting instead of planning.
ERP or accounting systems are underused.
Reports are too detailed but not useful.
Board or lender reporting is stressful.
Growth is happening, but financial clarity is not keeping up.
These are not just accounting problems. They are leadership problems.
The Future of Healthcare Finance Requires Better Systems and Better Leadership
Healthcare is not getting simpler.
Costs are rising. Reimbursement pressure continues. Staffing remains challenging. Technology expectations are increasing. Leaders are expected to move faster while managing more complexity.
In that environment, financial leadership is not optional.
Practices, clinics, and healthcare organizations need more than someone entering transactions and closing the books. They need a financial partner who can help connect systems, reporting, operations, and strategy.
The organizations that build financial clarity now will be better prepared to grow, adapt, and make confident decisions.
The organizations that delay may continue operating with late reports, unclear margins, disconnected systems, and avoidable financial stress.
How Team Consulting 360 Helps
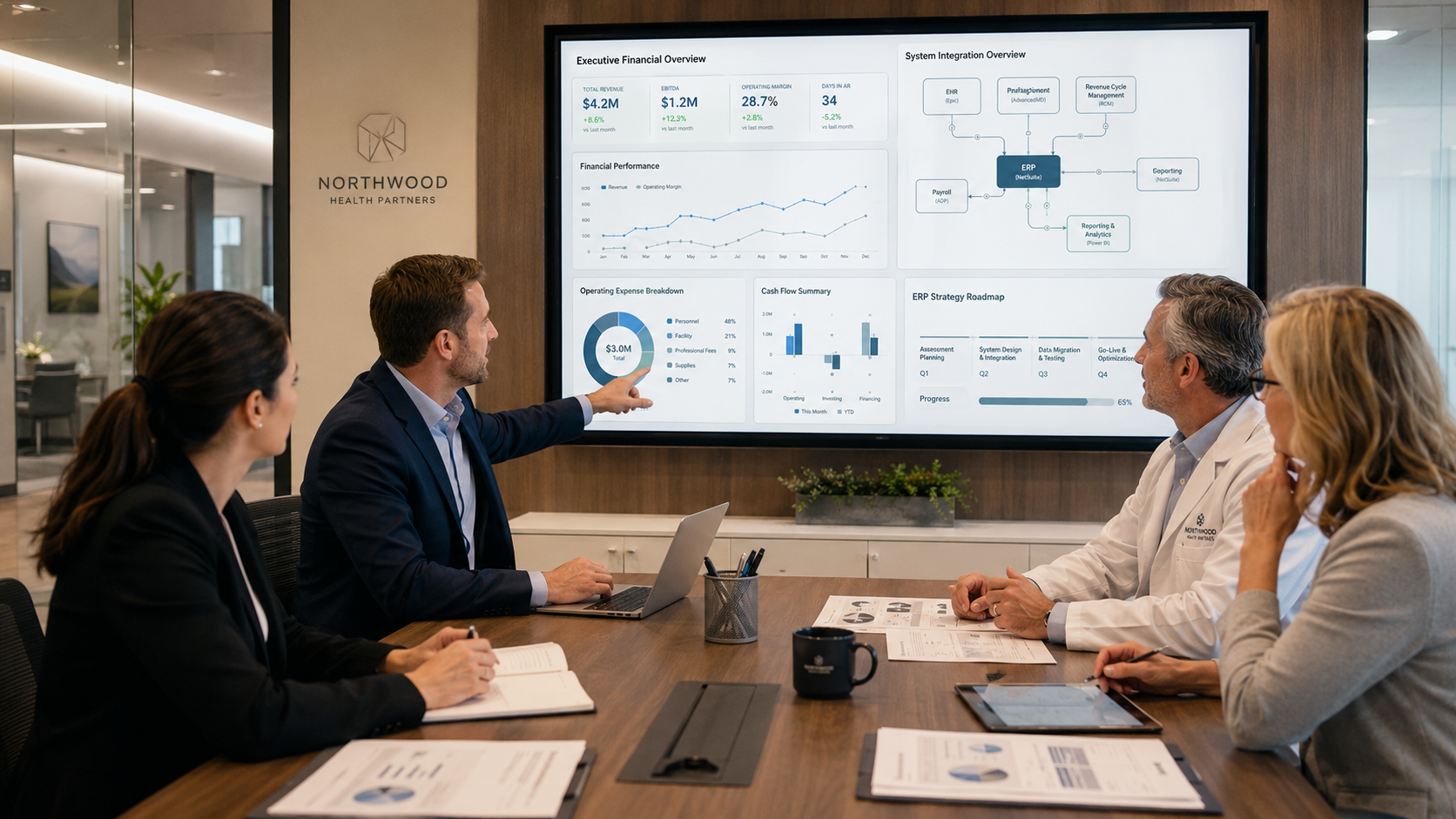
Team Consulting 360 helps organizations move from financial confusion to financial clarity.
For healthcare practices, clinics, nonprofits, and growing organizations, that means helping leadership strengthen reporting, improve financial systems, optimize processes, and build a more reliable foundation for decision-making.
Whether your organization needs fractional CFO advisory, ERP implementation support, financial reporting improvement, or process optimization, the goal is the same:
Give leadership timely, essential, aligned, and measurable financial information.
That is how healthcare organizations move from reacting to leading.
Final Takeaway
Healthcare organizations exist to serve people. But to serve people well over the long term, they need financial clarity.
Practices need it.
Clinics need it.
Large healthcare organizations need it.
Nonprofit healthcare organizations need it.
Financial leadership helps healthcare leaders understand the numbers, trust the reports, manage cash flow, improve systems, and make better decisions.
In today’s healthcare environment, financial leadership is no longer a luxury. It is part of building a stronger, more sustainable organization.
Reach out to Us
If your healthcare practice, clinic, or organization is relying on delayed reports, disconnected systems, or spreadsheets that no longer support your growth, Team Consulting 360 can help.
Schedule a financial leadership consultation with Team Consulting 360 and start building the clarity your organization needs to make better decisions.
Frequently Asked Questions
What is financial leadership in healthcare?
Financial leadership in healthcare is the strategic management of financial reporting, cash flow, budgeting, forecasting, systems, KPIs, and decision support. It goes beyond bookkeeping by helping leaders understand what the numbers mean and what actions should follow.
Do small medical practices need financial leadership?
Yes. Small medical practices often need financial leadership because they have limited margin for error. Cash flow, staffing costs, reimbursements, billing delays, and overhead can quickly affect profitability if they are not monitored properly.
What does a fractional CFO do for a healthcare organization?
A fractional CFO provides part-time executive financial leadership. For a healthcare organization, this may include budgeting, forecasting, cash flow planning, financial reporting, ERP support, KPI dashboards, board reporting, and strategic decision support.
Why do clinics struggle with financial reporting?
Clinics often struggle with financial reporting because data may be spread across billing systems, payroll systems, accounting software, scheduling platforms, and spreadsheets. Without integration and clear processes, reports can become delayed or unreliable.
How can ERP systems help healthcare organizations?

ERP systems can help healthcare organizations centralize financial data, improve reporting, reduce manual work, strengthen internal controls, and give leadership better visibility into performance. The key is implementing the system around real business decisions, not just software features.

